Historically, safe water interventions have focussed on providing improved water sources. However, there is now growing consensus among the WatSan community that water can be contaminated during transportation and storage in the home, even if water from the sources is safe (Clasen, 2003). A comprehensive safe water intervention should therefore begin with an improved water supply and be followed by safe handling of water in transport and storage. Household water treatment and safe storage (HWTS) is one option for safe handling of water. HWTS can also effectively treat water from unsafe sources.
This technical brief presents information on the current HTWS options. It is intended to assist field staff to select the most appropriate HWTS option for communities where HWTS has been determined to be the appropriate intervention. As the effectiveness of HWTS relies extensively on user acceptance, it is critical that users are involved in the HWTS option decision-making process, and are aware of how and why to use, maintain, and manage their HWTS option. In addition, all water supply and treatment interventions should be coupled with promotion activities to encourage proper handwashing and environmental hygiene in the home.
Introduction
The main objective of a HWTS intervention is to prevent waterborne transmission of diarrhoeal disease. This is especially important for children under five, who experience a large proportion of worldwide diarrhoeal disease morbidity and mortality, and for people with suppressed immune systems such as persons living with HIV and AIDS.
Programmes working to provide safe drinking water are beginning to focus on reducing or preventing contamination throughout the water chain, from source to the point of consumption. This is based on years of comprehensive research which has shown HTWS interventions are effective at reducing diarrhoeal disease incidence.

(WHO / Pierre Virot)
It is not always necessary to include HWTS in the safe water provision chain – it is only appropriate when the water source is of a dubious quality, or the water transport and storage conditions are unhygienic. If the source is known to be safe, the water can potentially be kept free from re-contamination by promoting safe transport and storage of water, and, if necessary, providing safe water storage containers.
However, if the source water quality cannot be guaranteed or the transport and storage conditions are unhygienic, the water should be treated before drinking. Treated water should then be protected against recontamination by: taking the water directly from the treatment unit; storing it in a safe storage container; and/or ensuring the presence of a chemical residual.
This technical brief summarises the stages of the safe water chain from source to consumption. The brief begins with a discussion on safe handling of water in transport and storage, and continues with a description of each of the seven HWTS options. The HWTS descriptions include information on the effectiveness, cost, operations and maintenance requirements, and benefits and drawbacks of each option. Programme experiences in emergency situations are highlighted in boxes throughout the text.
Seven HWTS options will be described in this brief. The first two are traditional methods to treat water. Although neither is yet proven to reduce diarrhoeal disease in users in developing countries, both can be effective at reducing microbial contamination in water (Clasen, 2008; Kotlarz, Submitted).
- Boiling
- Natural filtration and flocculation methods (sedimentation, cloth filtration, sand filtration, moringa seeds, alum)
The next five HWTS options that will be discussed are widely promoted and proven to reduce diarrhoeal disease in users in developing countries (Lantagne, 2006; Sobsey, 2008):
- Flocculation/disinfection sachets (including PuR® and WaterMaker®)
- Ceramic filtration (including pot- and candle-style filters)
- Biosand filtration
- Solar disinfection (SODIS)
- Chlorination (including tablets or liquid)
The ideal requirements for a successful HWTS programme are detailed in Box 1.
The option selected is:
- Effective at:
- removing waterborne pathogens of concern
- storing treated water safely in a container that can be cleaned
- reducing diarrhoeal disease incidence
- Appropriate for local conditions and water quality
- Acceptable to the user and consumers
The programme includes:
- Training on use and maintenance
- Regular monitoring of household water quality and use
- Provision for replacement parts
In the longer term, the option should be affordable to the users and replacement parts should be available locally.
A summary of the HWTS options is presented on the page after next in Table 1. This summary is intended to assist field staff to determine which option(s) might be appropriate in different settings. For turbid water, natural filtration or flocculation methods can be used prior to treatment to improve the visual quality of the water and, potentially, increase the efficacy and acceptability of the HWTS option. Boiling is not included in the table as a recommended option due to the drawbacks detailed in this brief.
Table 1: Household treatment and health promotion options in different settings
| Scenario | Diarrhoea outbreak or high risk? | Household Water Hardware Intervention | Public Health Promotion Intervention |
| Centralised water distribution system with chlorine residual (Camp setting) | No | Safe water collection and storage containers Check chlorine levels | Safe collection and storage |
| Yes | Check chlorine levels AND / OR Mass super chlorination of jerry can / storage containers | Safe collection and storage Sensitisation on use of chlorine | |
| <5NTU water from taps or protected source but no chlorine residual(Multiple sources) | No | Safe water collection and storage containers | Safe collection and storage |
| Yes | Short term: Household water chlorination (with tablets or liquid) If camp setting: Mass super chlorination of jerry can / storage containers | Sensitisation and training on use of chlorine | |
| Longer term (select one of): Sodis (if in village or camp with corrugated iron roofs and sun) OR Ceramic pot filters (if existing in-country experience) OR Ceramic Candle filters (preferably if spare parts available locally) OR Biosand filters + safe collection and storage containers AND If camp situation, Periodic super chlorination of jerry can / storage containers | O&M training + Safe collection and storage (especially Biosand) Sensitisation on use of chlorine | ||
| >5NTU waterfrom taps or protected source but no chlorine residual(Multiple sources) | No | Short term:Safe water collection and storage containers AND/OR Explore locally available flocculants and coagulants e.g. alum, natural coagulants | Safe water collection andstorage Correct use and safe disposal of coagulant |
| Longer term (select one of):Ceramic pots filters (if existing in-country experience) OR Ceramic Candle filters (preferably if spare parts available locally) OR Biosand filters + Safe water collection and storage containers | O&M training + Safe collection and storage (especially Biosand) | ||
| Yes | Short term:If available: PUR® / WaterMaker type sachets If not: Sedimentation (with provision of water storage containers if necessary) + household water chlorination (with tablets or liquid) | Correct use and safe disposal of coagulant + sensitisation on taste Sensitisation and training on sedimentation practices + use of chlorine | |
| Longer term (select one of): Ceramic Pots (if existing in-country experience) OR Ceramic Candle filters (preferably if spare parts available locally) OR Biosand filters + Safe water collection and storage containers AND If camp situation, Periodic super chlorination of jerry can / storage containers | O&M training + Safe collection and storage (especially Biosand) Sensitisation on use of chlorine |
Safe Water Handling: Transport and Storage
Safe water handling can prevent contamination that occurs between the source and the point of consumption. Water can be contaminated at the source itself, and/or become more contaminated when exposed to unclean containers, unclean hands, or environmental contamination during transport and storage. The contamination in transport and storage can be prevented through the use of safe containers, hygiene practices, and water treatment. As a discussion of interventions to maintain the safety of water sources is outside the scope of this document, this first section of the brief will describe safe container and hygiene practice strategies to prevent contamination. The following sections will describe the different HWTS options for water treatment.
The key safe container and hygiene practice strategies for preventing contamination are:
- Use of safe water transport and storage containers;
- Regular cleaning transport and storage containers;
- Not contacting water with unclean hands; and,
- Use of clean cups for drinking.
Safe Water Transport and Storage Containers
Containers used to transport and store water in different areas of the world range from traditional pots or urns made from natural materials such as gourds or clay, to metal containers made of steel, copper or aluminium, to, increasingly, recycled plastic jerry cans or new plastic buckets. In some areas, separate containers are preferred for transport and storage, such as easy to carry, lightweight plastic containers for transport followed by a ceramic container that cools the water for storage at the household level. In other areas, the same container is used for transport and storage.
The use of transport and storage containers with the following criteria will assist in reducing contamination:
- A small opening or lid that discourages users from placing potentially contaminated items such as hands, cups, or ladles into the stored water;
- A spigot or small opening to allow easy and safe access to the water without inserting hands or objects into the container;
- Instructions that are permanently attached for treating water and cleaning the container; and,
- Durability and acceptability to the user for water storage and transport.
In emergencies, containers for collecting and storing water are required immediately. As per the Sphere Standards (SPHERE, 2004), Oxfam recommends that “each household has at least two clean water collecting containers of 10-20 litres, plus enough clean water storage containers to ensure there is always water in the household.” To determine the appropriate safe storage container, first identify the containers currently being used, and determine if the containers are safe, or could be modified to be safe storage containers. Ideally, families should have separate containers for collection and storage of high-quality water (drinking, cooking) and household water (washing, cleaning, and hygiene) to reduce potential contamination. If closed, lidded containers are not available, efforts should be made to educate users to access the water by pouring from the container rather than dipping into the container with a potentially contaminated object.




The use of improved buckets alone has been shown to reduce diarrhoeal disease and improve water quality. “Analysis of water samples demonstrated that there was a 69% reduction in the geometric mean of faecal coliform levels in household water and 31% less diarrhoeal disease (P = 0.06) in children under 5 years of age among the group using the improved bucket. Regression models examining diarrhoea among under 5-year-olds confirmed the protective effect of the bucket and found that visible faeces in the family latrine and the presence of animals were significantly associated with an increased diarrhoeal incidence in children.
Although Oxfam advocates the use of locally-available transport and storage containers, it is recognised not all local containers are adequate. Thus, over the years Oxfam has designed and field-tested the Oxfam Bucket to be a practical, importable safe water container (Box 2). The design is now widely used by many agencies in emergency response.
The Oxfam Bucket was designed for use in emergency situations, and has the following characteristics:
- The lid is tight fitting with a capped opening to discourage hand contact during collection and transport. The cap is attached to the lid to prevent loss. The lid can be removed for cleaning.
- The tap is hygienically sealed with a push-tap.
- Where the walls meet the base, the bucket is curved to enable cleaning.
- The bucket is stackable, with one pallet containing 200 buckets.
- The bucket made of durable UV-resistant plastic, and is easy and safe to carry on the head.
There are two models of the Oxfam Bucket available in the Oxfam logistics catalogue: (1) a 14-litre bucket without a tap for collecting and transporting water (Code TWCT/2); and, (2) a 14-litre bucket with a tap for safely dispensing water and for use as a handwashing station (Code TWCT/1).


Keeping water storage containers clean
The second strategy to prevent contamination between source and point of consumption is to clean the transport and storage containers regularly – either once a week or whenever they appear dirty. The steps for cleaning are:
- Drain the container.
- Scrub the inside of the container using an abrasive (soft bristle broom, cleaning rag, small stones) and a cleaning agent (solution of chlorinated water or soap and water). Clean the exterior of the container with a cloth and soap or chlorine solution, paying particular attention to the area around filling and discharge openings.
- Rinse container with clean drinking water to remove cleaning agent residue.
In addition to regular cleanings, in camps or densely populated settings, Oxfam recommends periodic super chlorination of all receptacles, an example of which is presented in Box 3.
In June 2004, an outbreak of shigellosis was confirmed in Abou Shouk camp in the Northern Darfur province of Sudan. As water testing at the source showed no contamination, it was assumed that post-collection contamination was happening. The decision was taken to launch a programme of mass disinfection of all water containers in order to break the contamination cycle.
Five percent chlorine solution was used to clean containers. Approximately 100–150 millilitres were added to every container, along with some small stones. The container was shaken vigorously if it was closed or scrubbed with a local straw broom if open.
Diarrhoea figures from the clinics showed a fall in cases following the disinfection campaign; although it is difficult to collect statistically rigorous data it does appear that the campaign had an impact on the prevalence of watery and bloody diarrhoea.
Preventing contacting water with unclean hands and Using clean cups for drinking
The remaining two strategies to prevent contamination between source and point of consumption are both related to hygiene practices in the home. Potential for contamination will be reduced if hands are kept clean before handling of the water and if cups or mugs used for drinking are clean.
Summary
Using safe water transport and storage containers, regularly cleaning transport and storage containers, preventing water from contact with unclean hands, and using clean cups for drinking all can reduce the potential for contamination between source and point of consumption. If the source of water is known to be safe, the water can potentially be kept free from re-contamination by promoting these safe water handling measures, and, if necessary, providing safe water storage containers.
Safe Water Handling: Household Water Treatment and Safe Storage (HWTS)
If the source water quality cannot be guaranteed or the transport and storage conditions are unhygienic, water should be treated at the household level before consumption. When choosing which HWTS option to select in the situation you are working within, there are four main questions to consider:
- What options are available?
- What options are acceptable to the users?
- How serious is the diarrhoea risk in the intervention area?
- What options are appropriate for the water quality in the intervention area?
Questions 1, 2, and 3 can only be answered locally and general guidelines cannot be provided. However, it is possible to develop general guidelines for which options are appropriate for water quality characteristics, predominantly based on turbidity. HWTS options that are effective at three turbidity ranges are highlighted in blue Table 2.
| Boiling | Flocculant / disinfectant powders | Natural filtration / flocculation + disinfection | Chlorine solution | SODIS | Ceramic / Biosand Filtration | |
| Very turbid waters (>100 NTU) | Blue | Blue | Blue | |||
| Turbid waters (5-10 to 100 NTU) | Blue | Blue | Blue | Double dose | Blue | Blue |
| Low turbidity waters (<5-10 NTU) | Blue | Blue | Single dose | Blue | Blue |
Arsenic and fluoride are two water quality parameters of concern in many areas of the world. The only HWTS options that remove arsenic are flocculant/disinfectant powders and solar disinfection with lemon juice added. A modified version of the Biosand Filters, called the Kanchan Filter, has shown some promise at removing arsenic in some areas, but not in others. Fluoride is even more difficult to remove than arsenic, and none of the above options effectively remove fluoride. Water can be filtered through bone char at the household level to remove fluoride, although it is recommended that, if possible, an alternative source of water be located rather than attempt to treat fluoride at the household level.
The appropriate HWTS option can be selected for the area in which you are working by comparing the effective options for the water quality with the acceptable and available options in the area. All water treated with a HWTS option should then be protected against recontamination by: taking the water directly from the treatment unit; storing it in a safe storage container; and/or ensuring the presence of a chemical residual. Water quality interventions should always be a holistic intervention that focuses on creating an enabling environment to practice safe hygiene.
In the following section, information on the effectiveness, cost, operations and maintenance requirements, and benefits and drawbacks of each HWTS option is presented. Much of the information presented on each HWTS option is taken directly from the CDC/USAID fact sheets on HWTS, which can be found at www.ehproject.org/ehkm/pou_bib2.html (EHP, 2008). Experience with the HWTS options from programmes in emergencies is presented in boxes throughout the text.
HWTS Option 1: Boiling
Boiling is an ancient method of treating water and is currently common practice in some parts of the world. Over the years many organizations have extensively promoted boiling. However, boiling has serious drawbacks, including the expense, use of fuel, and association with higher levels of burn accidents and respiratory infections, especially among young children. For these reasons, Oxfam’s position is that boiling is not recommended as the optimum HWTS option. However, in areas where boiling is commonplace (as in many parts of Asia), and other HWTS options are limited, boiling can be promoted. Boiling promotion should focus on promoting the correct usage (1 minute of continuous boiling), safe storage of the boiled water, and practicing boiling as safely as possible.
Effectiveness
Effective boiling can inactivate all the bacteria, viruses, and protozoa that cause diarrhoeal disease (Clasen, 2008). However, studies in developing countries have documented incomplete inactivation of bacteria in boiled waters (Gupta, 2007). This disparity between laboratory and field results is attributed to users not heating the water to the boiling point and/or recontamination of boiled water in storage. To date, there have been no peer-reviewed studies assessing the health impact associated with boiling water, although some case-control studies in cholera outbreaks have noted boiling as protective against cholera (CDC, unpublished data).
Cost

The cost of boiling depends on the cost of the fuel source. In areas of the world where fuel is in short supply, boiling can be an expensive and environmentally damaging practice, in addition to being time consuming and taking the collector (often women) away from other productive work. In areas of the world with good fuel supply, boiling can be cost-competitive with other HWTS options. A recent study found the cost of boiling to be 0.272-1.68 USD/month in Vietnam, representing 0.48-1.04% of household income (Clasen, 2008).
Operation and Maintenance
Although boiling time recommendations vary significantly (range 0-20 minutes), in order to ensure water is safe for consumption the water simply must reach the boiling point of 100 C. The World Health Organization thus recommends that water be heated until it reaches the boiling point. Some organizations, such as the Centers for Disease Control and Prevention, recommend a continous boil of 1 minute, in order to ensure that users do not stop heating the water before the boiling point is reached. Boiling messages should focus on the appropriate time to boil water for, and the safe handling and storage of the water. It is recommended that water be stored in the container in which it was boiled, preferably a closed container with a lid, and that safe boiling practices and fire safety should be emphasised.
| Advantages | Limitations |
| Common knowledge and practice in many places Proven inactivation of all waterborne disease-causing organisms, even in turbid or contaminated water Existing presence in the household of all materials necessary to boil water | Lack of residual protection leaves boiled water vulnerable to recontamination Does not remove suspended or dissolved compounds Relatively high cost for fuel source and/or the opportunity cost of collecting fuel Concerns for environmental sustainability Leading cause of burns, especially in children Effects of indoor air pollution from cooking with biomass are associated with reduced birth weight, respiratory infections, anaemia, and stunting Lack of proven health impact Potential user taste objections Potential for incomplete water treatment if users do not bring water to full boiling temperature |
HWTS Option 2: Natural Filtration and Flocculation Methods
Although the following five natural filtration and flooculation options are not proven to reduce diarrhoeal disease incidence on their own, they can be used to pre-treat water before the use of proven household water treatment products to remove the particles and reduce the turbidity. These pre-treatment methods may also increase the efficacy of household water treatment products by removing materials that interfere with disinfection and physical filtration processes.
A simple option to pre-treat turbid water is to filter through a locally-available cloth. Users pour water from the transport container through the cloth into the storage container. The benefits of this option include its simplicity, the wide availability of cloth, and the fact that filtration through multiple layers of sari cloth has been proven to reduce cholera transmission in Bangladesh.

(CDC, R. Quick)
Settling and decanting is a method to reduce turbidity by letting the water sit for 2-24 hours so that the particulates settle to the bottom of the container. The clear water is then decanted off the top into a second container. The benefit of settling and decanting is that it requires no equipment besides the containers. The drawbacks of settling and decanting are the need for two-three containers, the time it takes the water to settle, and, if the containers are opaque, the difficulty in observing the effect of settling. In laboratory studies, the use of settling and decanting significantly reduced the turbidity of water, and also significantly reduced the disinfectant demand of turbid waters.
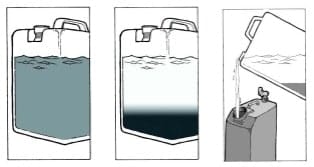
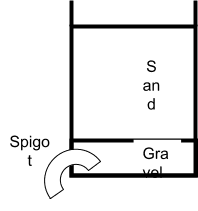
Filtration through sand is a fast and simple pre-treatment option. Users pour water from a transport container through a container of sand with gravel and a spigot at the bottom. The water then flows into a storage container. The benefits of sand filtration are that it is effective at removing some bacteria, it is simple and fast for the user, and, if sand is available locally, it is inexpensive. The drawback of sand filtration is that it requires three containers and a spigot. In laboratory studies, the use of sand filtration significantly reduced the turbidity of water, and also significantly reduced the disinfectant demand of turbid waters.
The moringa tree pod contains a seed which, when crushed, is a natural flocculant. Users pick and dry the pods, and then remove the seeds. The seeds are shelled, crushed using a mortar and pestle, and then about 2 grams of the seeds are added to 20 litres of water. The water is stirred for five minutes, and users let the moringa settle for 24 hours before decanting it off into another container. The benefits of moringa are that it is an effective flocculant. The drawbacks of the use of moringa as a pre-treatment option are that it is time- and labor-intensive, the dosing of moringa varies for different water, and the moringa flavor may be objectionable. In laboratory studies, the use of moringa significantly reduced the turbidity of water, but also significantly increased the disinfectant demand of turbid waters.

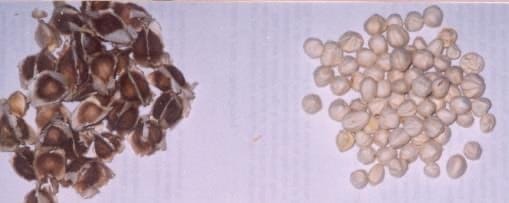

Shelled and unshelled seeds (CDC, D. Lantagne)
Aluminum sulfate is widely used as a flocculant in water treatment plants in the United States and Europe. It is also widely available in developing countries, sold in blocks of soft white stone, and generally called ‘alum’. There are numerous ways to use alum as a flocculant, including to crush it into a powder before adding it to water, stirring, and decanting; or, stirring the whole stone in the water for a few seconds and waiting for the solids to settle. The benefits of alum are that it is widely available, is proven to reduce turbidity, and is inexpensive. The drawbacks of alum are that the necessary dosage varies unpredictably, and an overdose leads to a salty, unpalatable taste. In laboratory studies, the use of alum significantly reduced the turbidity of water, and also significantly reduced the disinfectant demand of turbid waters.

(CDC, D. Lantagne)
Operation and Maintenance
The materials and skills requirements for natural flocculation and filtration methods are minimal. Care should be taken in all of these methods to ensure solids are removed and the containers cleaned on a regular basis.
Advantages and Limitations
| Advantages | Limitations |
| Low cost and simple methods Reduction of turbidity for subsequent treatment Some options reduce disinfectant demand for subsequent treatment Clear water is generally more acceptable to the user | Do not produce microbiologically safe water Several containers are required Some options increase disinfectant demand The procedures can be labour intensive and take significant time |
HWTS Option 3: Flocculation/disinfection sachets
Combined flocculant/disinfectant sachets (such as PuR® and WaterMaker®) are contain powdered ferric or aluminium sulfate (flocculant) and calcium hypochlorite (a disinfectant). They are designed to reverse-engineer a water treatment plant, incorporating the multiple barrier processes of removal of particles and disinfection. PuR® is produced by the Procter & Gamble Company and has been distributed free of charge in a number of emergency settings. Flocculant/disinfectant sachets are available in the Oxfam equipment catalogue (Code FCF/1).
Effectiveness
PuR® has been proven to remove the vast majority of bacteria, viruses, and protozoa that cause waterborne disease, even in very turbid waters (Souter, 2003; Crump, 2004). PuR® has also been documented to reduce diarrhoeal disease from 16 to greater than 90% incidence in five randomized, controlled health intervention studies (Clasen, 2007). In addition, PuR® removes the majority of heavy metals, such as arsenic, and chemical contaminants, such as some pesticides, from water (Souter, 2003). Studies showing the efficacy of PuR® have been conducted in the laboratory and in developing countries, in rural and urban areas and refugee camps, and include adults and children that are poor and/or using highly turbid water.

(Procter & Gamble)
Operation and Maintenance
To treat water with PuR®, users open the sachet, add the contents to an open bucket containing 10 litres of water, stir for 5 minutes, let the solids settle to the bottom of the bucket, strain the water through a cotton cloth into a second container, and wait 20 minutes for the hypochlorite to inactivate the microorganisms. The residual chlorine protects treated water from recontamination. As flocculant/disinfectant powders are a consumable, a supply chain will need to be established to provide sufficient sachets to the users. In addition, the residue (floc) should be disposed of safely (ideally buried), which can be problematic in flooded areas.

(P&G, G. Allgood)
Cost
PuR® sachets are centrally produced in Pakistan, and sold to NGOs at a cost of 3.5 US cents per sachet. It is estimated that each sachet cost 10 US cents by the time it arrives at the user, for a total treatment cost of 100 USD per 10,000L of water treated.
Advantages and Limitations
| Advantages | Limitations |
| Proven reduction of bacteria, viruses, and protozoa in water Removal of heavy metals and pesticides Residual protection against contamination Proven health impact Acceptable to users due to visual improvement in the water Sachets are easily transported due to their small size, long shelf life, and classification as non-hazardous material for air shipment Reduced production of disinfection by-products because organic material is removed prior to disinfection (Lantagne, 2008) | Multiple steps are necessary to use the product, which requires a demonstration to teach new users The need for users to have, employ, and maintain two buckets, a cloth, and a stirring device The higher relative cost per litre of water treated compared to other household water treatment options Some resistance to colour/taste Residue is difficult to dispose of in flood-affected areas |
PuR® is the most extensively evaluated HWTS option in emergency situations. Procter & Gamble have worked to position PuR® as an appropriate and effective option for acute and long-term emergency situations. The efficacy of PuR® in reducing diarrhoeal disease incidence in refugee situations and the acceptability of PuR® in emergencies have been established in the peer-reviewed literature. There is also a standard operating procedure for implementing emergency programmes with PuR®.
In Monrovia, Liberia, a 12-week effectiveness study of PuR® use among 400 households was conducted in camps for displaced populations with epidemic diarrhoea during the rainy season. Each household was provided with 21 sachets of PuR® per week, an initial one-on-one training, and follow-up weekly visits for twelve weeks. Use of PuR® was high, with 95% of chlorine residual tests positive at the household level. Use of PuR® and improved storage was associated with a reduced diarrhoeal disease incidence of 90% and prevalence of 83%, when compared with control households with improved water storage alone.
A knowledge, attitudes, practices, and drinking water quality evaluation was conducted among 100 PuR® recipients four to six weeks after local leaders distributed PuR® free of charge to populations affected by Tropical Storm Jeanne in Haiti in September 2004. Water quality testing at the source and household was also completed. The results of the survey found 78% of respondents correctly answered five questions about how to use PuR®, 81% reported PuR® easy to use, and 97% reported PuR® treated water appears, tastes, and smells better than untreated water. However, only 22% reported using PuR® that day, and only 9% had correct chlorine residual levels at the time of testing. Despite the high acceptability reported in the survey, the following factors were concerning: the relatively low usage; the fact the future willingness to pay for the product was significantly less than the social marketing price in Haiti; and, emergency response NGOs in Haiti were not interested in distributing the product in the acute emergency phase due to competing demands, lack of familiarity with the product, and lack of training. As a result, thousands of sachets did not leave the warehouse for several weeks following the flooding, until the NGO Population Services International began the programme with local leaders distributing the sachets.
Subsequent programme evaluations of PuR® use in emergencies – with CARE in Haiti flooding and Ethiopia nutrition projects, with Samaritan’s Purse in IDP camps in Uganda, and with UNICEF in response to flooding in Bangladesh – have identified the following important factors for programme success:
- The availability of all the necessary hardware to use PuR®, including strong containers and stirrers;
- The critical need for initial and follow-up training to teach people to use the product correctly, answer questions, and address concerns; and,
- The need to use PuR® in “stable” emergencies, where staff can focus on the training necessary.
The standard operating procedures (SOP) for distributing PuR® in emergency situations identify the following five main obstacles that should be carefully addressed to achieve a successful programme:
- Lack of familiarity with the product and its usage, resulting in misperceptions of labour and time demand, and associated logistical challenges;
- Chlorine odour and taste;
- Colour change during treatment process;
- Lack of available buckets and cloth; and,
- Acceptance by government officials and community leaders.
The SOP details how to overcome these obstacles and concludes: “experience with PUR in a variety of emergency relief situations has shown that by addressing these obstacles with a team of trainers, emergency relief groups can successfully distribute PUR.
HWTS Option 4: Ceramic Filtration
Locally manufactured ceramic filters have traditionally been used throughout the world to treat household water. Today, numerous locally made and commercial HWTS ceramic filters are widely available in developed and developing countries. One commercial candle filter, the Stefani filter, is stocked in the Oxfam equipment catalogue, as: (1) a complete set with a bucket, 2 candles, a tap, and a pictorial leaflet (Code FHF/1); or, (2) a set for when a local container is available, only including three candles and a tap (Code FHFCT/1).


Effectiveness
The effectiveness of ceramic filters at removing bacteria, viruses, and protozoa depends on the production quality of the ceramic filter. Most ceramic filters are effective at removing most of the larger protozoal and bacterial organisms, but not at removing the smaller viral organisms (Lantagne, 2001). Studies have shown removal of bacterial pathogens in water filtered through high quality locally-produced and imported ceramic filters in developing countries (Clasen, 2004). A 60-70% reduction in diarrhoeal disease incidence has been documented in users of these filters (Clasen, 2007). Studies have also shown significant bacterial contamination when poor-quality locally produced filters are used, or the receptacle is contaminated at the household level (Lantagne, 2001). Because of the lack of residual protection, it is important that users be trained to properly care for and maintain the ceramic filter and receptacle.
Costs
A candle filter unit generally costs 15 USD. Each unit treats about 20,000L, costing 7.50 USD per 10,000L of water treated. Unit costs for locally made ceramic filters range from 7.50-30 USD depending on the manufacturing country.

Operation and Maintenance
To use the ceramic filters, families fill the top receptacle or the ceramic filter itself with water, which flows through the ceramic filter or filters into a storage receptacle. Contaminants are mechanically trapped in the pores in the ceramic or removed by silver imbedded in the ceramic. The treated water is then accessed via a spigot embedded within the water storage receptacle. Over time the filter can become clogged with debris, which blocks the pores in the ceramic and causes the flow rate to decrease from the optimal rate of 1-3 litres per hour. The ceramic candles can be cleaned by gently scrubbing the surface using a soft brush, and then rinsing with water. The receptacle should be cleaned using filtered or disinfected water.
Advantages and Limitations
| Advantages | Limitations |
| Proven reduction of bacteria and protozoa in water Acceptability to users because of the simplicity of use Proven reduction of diarrhoeal disease incidence in users Long life if the filter remains unbroken A low one-time cost Perceived as a valuable asset by the users Pot-style filters can be produced locally and supports local craftsmen and supply chain | Lower effectiveness against viruses Lack of residual protection can lead to recontamination if treated water is stored unsafely Variability in quality control of locally produced filters Filter breakage over time, and need for spare parts Filters and receptacles need to be regularly cleaned, especially when using turbid source waters A low flow rate of 1-3 litres per hour Unlikely to be appropriate in first phase emergency response due to need for user education, follow-up and supply chain establishment Difficult to transport |
Oxfam has been involved in the distribution and evaluation of ceramic filters in emergency situations in numerous countries. Two examples, from Sri Lanka after the tsunami and the DR after flooding, will be described here.
In response to the December 2004 tsunami, both Oxfam and the American Red Cross (ARC) distributed ceramic filters. Oxfam distributed candle filters three months after the tsunami in Galle to people moving out of emergency camps with little filter training, and in Trincomalee six months after the tsunami to people moving into transitional shelters with good training. ARC distributed locally-made pot filters six months after the tsunami to people in Weligama moving back into their homes, with good training. An evaluation to assess acceptability was conducted six months after the tsunami – three months after distribution of the filters in Galle, and 1-2 weeks after distribution in Trincomalee and Weligama.
The evaluation found only 23% of people in Galle had sufficient filtered water to fill a cup at the time of the household visit, in contrast to 79% in Trincomalee and 96% in Weligama. Factors associated with higher levels of use included: having used wells as opposed to piped water as a source of drinking water before the tsunami, future planned well use, practising any type of water treatment, a greater length of time since the tsunami, higher quality of living shelter, higher intensity of programmatic support, and the distribution of pot as opposed to candle filters. Barriers to use were insufficient filter training and lack of living space. The evaluation concluded “filters were well received among recipients living in transitional and permanent shelters who received adequate programmatic support. However, filters should not be given out in the acute stages of an emergency response when internally displaced persons are living in emergency shelters and distributing organizations have too few resources to spend on ensuring high levels of use and correct use.”
The abstract of a second evaluation of an Oxfam ceramic filter emergency implementation follows. As part of its response to flooding in the Dominican Republic in 2003, Oxfam GB distributed ceramic “candle” water filters to householders in 7 affected communities. In a randomized, controlled trial conducted among 80 householders in one community during the six-month design life of the ceramic filter elements, faecal water contamination was consistently lower among intervention households than control households (geometric mean themotolerant coliform (TTC) of 2.9/100 ml vs 32.9/100 ml, p<0.0001). Overall, 70.6% of samples from the intervention households met WHO guidelines for zero TTC/100 ml compared to 31.8% for control households (p < 0.001). A cross-sectional study 16 months following filter distribution revealed that 88.7% of the filters were still in the recipient households; 48.7% were still operating properly, the others failing mainly due to breakage, clogging or expiration of the useful life of the candle elements. While source waters were still highly contaminated, 54% of samples from working filters were free of TTC. These results suggest that ceramic water filters can be an effective intervention for providing populations affected by disasters with safe drinking water during resettlement. They may also be a potentially sustainable long-term solution, provided householders have access to affordable replacement filter elements. While training was found to be “vital” to programme success, it was determined the training did not have to be “extensive.”
Based on these evaluations, it is recommended that all recipients of ceramic filters receive practical and participatory training that includes information on: the purpose of the filter; preparing candles; assembling and using the water filter; building a stand; determining when the filter needs to be cleaned; and cleaning the candles and the buckets. Detailed work plans and promotional materials are provided on the CD that accompanies this brief.
Are ceramic filters an appropriate response in emergencies?
Field staff have raised the question of whether it is appropriate to distribute ceramic filters in emergency settings when replacement filter supplies cannot be guaranteed. Whilst the ideal is to distribute treatment technologies that are sustainable in the long term and create access to markets for replacement parts, a single distribution of ceramic water filters can provide safe water for recipients for up to two years. In most cases, this is sufficient time to cover the risky post-emergency period.
That being said, the immediate emergency environment is not always favourable for filter distribution. Filters are more likely to be appropriate post-emergency or in longer-term response when the time can be dedicated to operation and maintenance, training, and monitoring. Some questions to consider when determining whether to distribute ceramic filters include:
- If there is a centralised water supply system, what is the added value of distributing filters?
- If the setting is a rapid emergency, is a simpler water treatment alternative available?
- Are ceramic filters a familiar technology in the area and are replacement supplies locally available?
- Have locally-made ceramic filters passed microbiological testing and quality control checks?
- Do recipients have space in their dwellings to store the filter?
- Do project staff have time to train users and complete follow-up monitoring?
Field staff in each particular setting will need to determine first whether ceramic filters should be distributed, and secondly whether the programme will aim for distribution for treatment in the emergency period only or whether to create sustainable access to ceramic filtration for long-term household water treatment.
HWTS Option 5: BioSand Filtration
The BioSand Filter (BSF) is a slow-sand filter adapted for use in the home. The version of the BSF most widely implemented consists of layers of sand and gravel in a concrete or plastic container approximately 0.9 meters tall, and 0.3 meters square. The water level is maintained to 5-6 cm above the sand layer by setting the height of the outlet pipe. This shallow water layer allows a bioactive layer to grow on top of the sand, which contributes to the reduction of disease-causing organisms. A diffuser plate with holes in it is placed on the top of the sand layer to prevent disruption of the biolayer when water is added to the system. BSFs are promoted by NGOs, such as the Centre for Affordable Water Supply (CAWST), Samaritan’s Purse, and Bushproof, who partner with local producers to make the filters and local distributors to provide the filters to the families. Training materials and information can be found at www.cawst.org, www.bushproof.org, or www.biosandfilter.org.
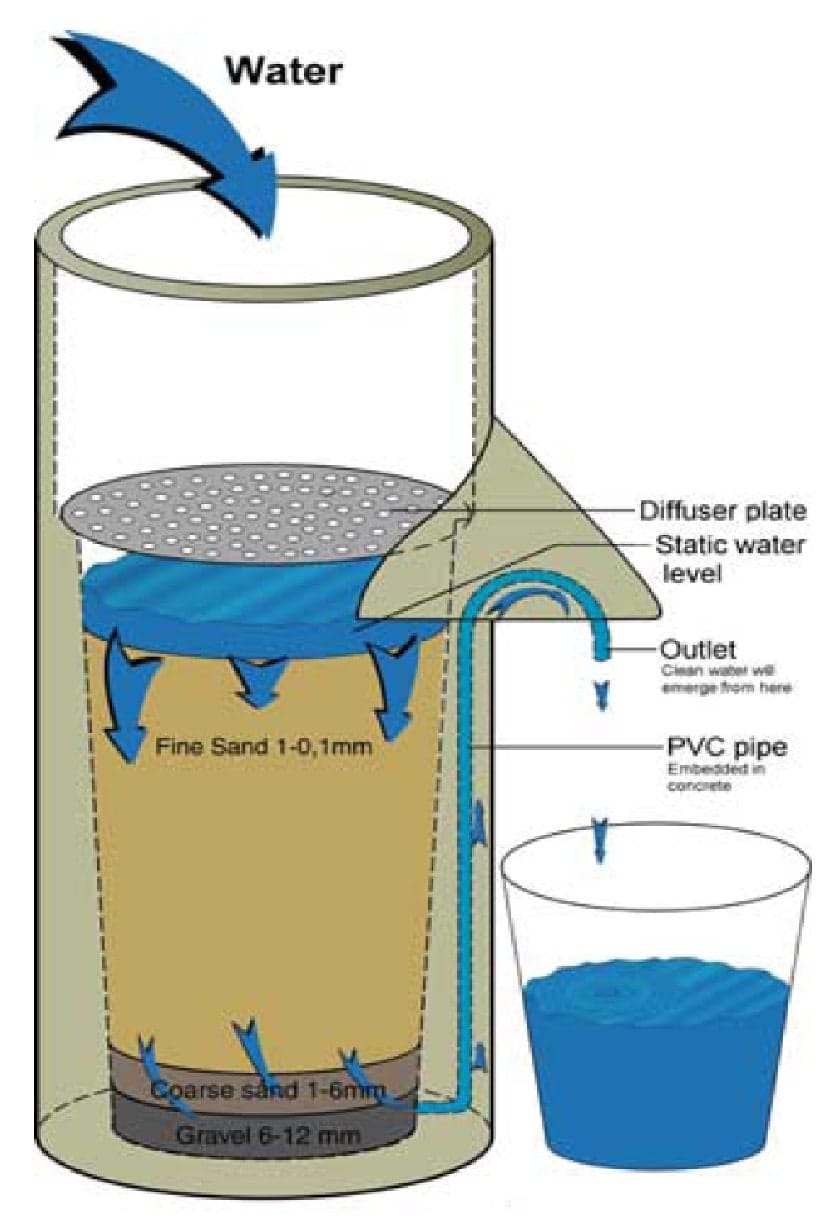
Effectiveness
In laboratory and field testing, the BSF consistently reduces bacteria by 81-100% and protozoa by 99.98-100% (Kaiser, 2002). Initial research has shown that the BSF removes less than 90% of indicator viruses. Although the data has not yet been published, initial data from the first diarrhoeal disease impact study on the BSF, conducted by the University of North Carolina, documented an estimated 40% reduction in diarrhoeal disease in users of the BSF. Three more health impact studies, in Ghana, Cambodia, and Honduras, are currently being planned.

(Pure Water for the World)
Cost
Each Biosand filter unit costs between 12-100 USD and can treat an unlimited volume of water. There are no recurrent costs and the lifetime of a unit can be many years.
Operation and Maintenance
To use the system, users simply pour water into the BSF, and collect finished water from the outlet pipe in a safe storage container. Biosand filters ideally produce 1 litre of water per minute. When the flow rate becomes unacceptably low, it is restored by a process called ‘wet harrowing’. Users fill the filter with water after blocking the spout, remove the diffuser plate, and swirl water around inside the filter without touching the sand. Blocked dirt will come into suspension, and the muddy water can be removed with a cup.
Advantages and Limitations
| Advantages | Limitations |
| Proven removal of protozoa and most bacteria Acceptability to users because of high flow rate, ease-of-use, and visual improvement in the water Production from locally available materials One-time installation with low maintenance requirements Long life Suitable for local production and opportunities for local business Evidence of long term use and performance | Sub-optimal removal of viruses Lack of residual protection or built in safe storage leaves water susceptible to recontamination Current lack of studies proving health impact Limited portability and difficult of transport due to heaviness of the filter and high up front cost |
HWTS Option 6: Solar Disinfection
Solar disinfection (SODIS) was developed in the 1980’s to inexpensively disinfect water used for oral rehydration solutions used to treat diarrhoea. In 1991, the Swiss Federal Institute for Environmental Science and Technology (SANDEC, EAWAG) began to investigate and implement SODIS as an HWTS option.

(SANDEC / EAWAG)
Effectiveness
In the laboratory, SODIS has been proven to inactivate the viruses, bacteria, and protozoa that cause diarrhoeal diseases (Mendez-Hermida, 2005; Berney, 2006). Field data have also shown reductions of bacteria in water from developing countries treated with SODIS (Rainey, 2005). In four randomized, controlled trials, SODIS has resulted in reductions in diarrhoeal disease incidence ranging from 9-86% (Clasen, 2007).
Cost
SODIS is essentially a zero-cost technology, although educational programming and the cost of the plastic bottles will need to be accounted for in programming costs for the intervention.

(SANDEC / EAWAG)
Operation and Maintenance
Users of SODIS fill 0.3-2.0 litre plastic soda bottles with low-turbidity water, shake them to oxygenate, and place the bottles on a roof or rack for 6 hours (if sunny) or 2 days (if cloudy). The combined effects of UV-induced DNA alteration, thermal inactivation, and photo-oxidative destruction inactivate disease-causing organisms. If drops of citric acid (lemon juice) are added this has been shown to reduce levels of arsenic.
Advantages and Limitations
| Advantages | Limitations |
| Proven reduction of viruses, bacteria, and protozoa in water Proven reduction of diarrhoeal disease incidence in users Acceptability to users because of the simplicity of use No cost to the user after obtaining the plastic bottles Minimal change in taste of the water Although SODIS does not have a chemical residual, recontamination is unlikely because water is served directly from the small, narrow-necked bottles with caps in which it is treated | The need for pretreatment (filtration or flocculation) of waters of higher turbidity User acceptability concerns because of the limited volume of water that can be treated at once and the length of time required to treat water The large supply of intact, clean, suitable plastic bottles required Difficult for the user to judge the range of factors which are required for adequate disinfection WatSan staff can oversimplify the method in trainings with users which can lead to users not adequately treating their water |
HWTS Option 7: Chlorination
Chemical disinfection with chlorine is the most common way to treat water at the household level. Three forms of chlorine are widely used in developing countries: (1) Mother solution (1% sodium hypochlorite solution made from calcium hypochlorite or bleach); (2) Dilute sodium hypochlorite specially packaged for water treatment in bottles (WaterGuard or Sûr’Eau): or, (3) Tabletted sodium dichloroisocyanurate (such as Medentech Aquatabs® – Code FPU in the Oxfam Equipment Catalogue). All are distributed with instructions detailing how much to add to a certain volume of water.

(PSI/Nigeria)
Effectiveness
At concentrations that are used in HWTS programmes – 2 mg/L for clear water, 4 mg/L for turbid water (Lantagne, in press) – chlorine is effective at inactivating most bacteria and viruses that cause diarrhoeal disease (CDC, 2008). However, it is not effective at inactivating some protozoa, such as Cryptosporidium. Numerous studies have shown complete removal of bacterial pathogens in chlorinated water in developing countries (Quick, 1999; Crump, 2004). In seven randomized, controlled trials, chlorination has resulted in reductions in diarrhoeal disease incidence in users ranging from 22-84% (Clasen, 2007). These studies have been conducted in rural and urban areas, and include adults and children that are poor, living with HIV, and/or using highly turbid water.
Operation and maintenance
Sodium hypochlorite solution is packaged in a bottle with directions instructing users to add one full bottle cap of the solution to clear water (or two caps to turbid water) in a standard-sized storage container, agitate, and wait 30 minutes before drinking. Aquatabs are packets in strips of ten tablets with directions instructing users to add one tablet to clear water (or two tablets to turbid water) in a standard-sized container, and wait 30 minutes before drinking. The residual chlorine protects treated water from recontamination. As all chlorination products are consumable, a supply chain will need to be established to provide sufficient sachets to the users. Care should be taken to ensure the right amount of liquid or tablets for the size of the collection container, and to keep both products out of the reach of children.
Cost
The cost of enough liquid socially marketed sodium hypochlorite solution to treat 1,000 litres of water ranges from 0.15-0.97 USD, with an average of 0.33 USD. The cost of chlorine tablets depends on the manufacturer and the size of the tablet, but generally is slightly higher than the cost of locally-made solution.
Advantages and Limitations
| Advantages | Limitations |
| Proven reduction of most bacteria and viruses in water Residual protection against contamination Acceptability to users because of ease-of-use Proven health impact Scalability, particularly in epidemic situations Low cost Readily available in most places | Relatively low protection against some viruses and parasites Lower disinfection effectiveness in turbid waters contaminated with organic and some inorganic compounds Potential user taste and odour objections Necessity of ensuring quality control of solution Unnecessary concern about the potential long-term carcinogenic effects of chlorination by-products (Lantagne, 2008) The need to have a constant supply chain for the consumable products |
Centralised and household-level chlorination are, arguably, the most commonly applied water quality interventions in emergency situations. However, there are few peer-reviewed studies assessing the efficacy of chlorination at the household level in emergencies, as “bucket chlorination” is a standard intervention that is assumed to be effective. The use of chlorine tablets, such as Aquatabs®, is also standard in many emergency responses. Three representative chlorination programmes will be discussed here: the use of Population Services International chlorination products in cholera response, bucket chlorination, and local generation of sodium hypochlorite.
Population Services International (PSI) socially markets small bottles of sodium hypochlorite in 19 countries. In 2007, PSI sold more than 12 million bottles of solution, treating over 12 billion litres of water. Using the socially marketed, locally produced product for cholera response has occurred since the first programme countries, when it was found that the product could be appropriate for cholera response, and that using the product for cholera response could stimulate demand for national sales. Five months after distribution, 33% of people confirmed the presence of chlorine residual in their drinking water. In 2007, PSI worked with emergency organizations in 12 countries to distribute over 2.3 million bottles of solution for cholera response.
During the 2006 cholera outbreak in Northern Uganda, the cholera task force stipulated that all drinking water should be collected from hand pumps and then chlorinated. People collecting water from the river during this time would be fined. Oxfam worked to train community health volunteers (CHVs) to add Aquatabs to jerry cans at each hand pump in the camp. Later, due to a shortage of Aquatabs, the CHVs were trained to safely make mother solution and administer doses of chlorine solution to each jerry can. Although the campaign was largely successful, challenges included:
- Compliance issues with mass chlorination, as people objected to the unfavourable taste;
- The common perception that eating Aquatabs would protect people from cholera and a lack of storage space in the house out of the reach of children; and,
- The difficulty in treating smaller quantities than 20 litres with Aquatabs.
These challenges were addressed by having only the CHVs add the Aquatabs or mother solution to water to ensure the correct dose and prevent ingestion. When the programme transferred to using mother solution, CHVs were able to adjust the dose for the container size.
The Jolivert Safe Water for Families (JSWF) Programme is a chlorination project in northern Haiti that began in September 2002 with 200 pilot project families. Chlorine solution is produced at the Jolivert Clinic using a hypochlorite generator. Families purchase this disinfectant in refillable 250 ml bottles either at the clinic (0.16 USD per bottle) or from 25 designated resellers throughout the surrounding towns and communities (0.20 USD per bottle, with the margin going to the reseller). Users add one capful to 5 gallons of water stored in a local container modified with a tap and lid. Three Haitian technicians produce the hypochlorite solution, offer trainings to bring new families into the program, conduct household visits to provide ongoing training and chlorine residual testing, sell the hypochlorite solution, and maintain records. All programme staff are fully paid from programme income. An independent evaluation of the pilot project in January 2003 documented a reduction in diarrhoeal disease incidence of 55% among users. Based on these successful results, the project began expanding, and now has over 4,000 families enrolled.
A study in 2007 found the determinants of hypochlorite use to vary among stages of adoption. Cost of the storage container is a barrier to entering the program, but cost of the solution is not a barrier to consistent use. Travel costs and time inhibit those in remote communities from using consistently. Lack of knowledge and self-efficacy are barriers to entry, and social support and social norms are determinants of all stages of adoption. Household visits by JSWF technicians appear to increase the rate of purchase. The Jolivert programme has been able to operate continuously through, and respond to, numerous emergencies – including floods, hurricanes, political upheaval, and riots – due to the local production and management, focus on training and follow-up with the users, and continued slow, steady growth.
Lastly, prior to concluding this brief, we would like to summarize two evaluations completed after the December 2004 tsunami that discuss emergency implementations of multiple HWTS interventions.
In The Drinking Water Response to the Indian Ocean Tsunami Including the Role of Household Water Treatment, authors Thomas Clasen and Lucy Smith summarise their findings from interviews and field visits that commenced eight weeks after the tsunami.
Despite evidence in development settings and certain emergencies that household water treatment, including chlorination, filtration, solar disinfection, and combined flocculation/disinfection, are effective in improving the microbiological quality of drinking water and thus preventing the risk of waterborne disease, household-based approaches did not play a significant role in the initial phases of the tsunami response, with the possible exception of boiling. This was not due to their lack of availability; millions of units of these products were shipped to the region. Rather, responders often found that household water treatment was not suitable during the immediate aftermath of the disaster due to:
- The need to emphasize water quantity over water quality,
- The unique conditions imposed by the tsunami that continued to necessitate the supply of bulk treated water,
- The unavailability of human and other resources for the programmatic support to launch household water treatment,
- Concerns that the introduction of new methods of water treatment would send mixed messages about other practices, and
- Concerns about the sustainability of such methods.
Boiling did play a role, though there was evidence to suggest that, as it was practised in tsunami-affected populations, boiling was not providing adequate protection against faecal contaminants. Some organizations expressed the view that household water treatment would be introduced during the resettlement phase of the disaster response.
These conclusions highlight the need for appropriate assessment prior to the initiation of HWTS programmes. HWTS options will not be appropriate in all emergencies, and understanding their appropriate role is key to successful implementations.
Five months after the tsunami, an evaluation in three Indonesian sub-districts in households who received free distribution of liquid sodium hypochlorite solution was conducted. Two sub-districts (Nias and Simeulue) were rural, island communities, and the third (Aceh Besar) comprised of temporary living camps and tent camps.
The survey found reported use of sodium hypochlorite to be 28%, 21%, and 12% in Aceh Besar, Nias, and Simeulue, respectively. Confirmed use of sodium hypochlorite, as measured by the presence of chlorine residual, was found to be 14%, 14.7%, and 2.64%, respectively. Factors found to be associated with decreased risk of E. coli contamination in stored water included:
- Reported use of sodium hypochlorite (Aceh Besar, Simeulue)
- Presence of free chlorine residual (Aceh Besar, Nias, Simeulue)
- Observed use of washing soap with hands (Simeulue)
- Use of a latrine (Simeulue)
Interestingly, use of a narrow-mouthed water storage container, reported boiling, adequate boiling, or adequate boiling with water storage were associated with decreased risk of E. coli in stored water. This evaluation highlighted the fact that not all interventions promoted (such as boiling) were effective at maintaining stored water quality, and, although there was low use of sodium hypochlorite, it was the only intervention effective in all sub-districts. In the community with the lowest use of sodium hypochlorite, handwashing with soap, and latrine use were also effective interventions.
Summary of HWTS in Emergencies for Oxfam
It is hoped that this technical brief is able to provide field staff with answers to questions they need to determine, if, and which, HWTS option to use in emergency circumstances. In summary, key points from the document are:
- HWTS is an appropriate intervention when water from the source is contaminated and/or it is not possible to ensure hygienic transport and storage of water.
- Although there is no one HWTS option appropriate for all circumstances, many of the options are appropriate in different circumstances. To determine which option is appropriate for the local circumstance, the following questions should be asked:
- What options are available?
- What options are acceptable to the users?
- How serious is the diarrhoea risk in the intervention area?
- What options are appropriate for the water quality in the intervention area?
- Successful HWTS programming depends on community acceptance and adoption, and user training is vital. Behaviour change communications and community involvement in the programme will greatly enhance the uptake and long-term sustainability of the HWTS intervention.
- Implementation materials and technical assistance to support on-the-ground implementers are vital. There is a wealth of health promotion materials that have been developed for HWTS. A CD that accompanies this technical brief has links to many of these.
We wish you the best in your programmes, and if you have any questions, please feel free to email Oxfam Headquarters or Daniele Lantagne at daniele.lantagne@lshtm.ac.uk.
References
The attached CD contains numerous helpful documents and links as well.
Aquaya (2005). Standard Operating Procedure for the Deployment of Procter & Gamble’s PUR Purifier of Water in Emergency Response Settings. San Francisco, CA, USA.
Berney, M., H. U. Weilenmann, et al. (2006). “Efficacy of solar disinfection of Escherichia coli, Shigella flexneri, Salmonella Typhimurium and Vibrio cholerae.” J Appl Microbiol 101(4): 828-36.
Brin, G. (2003). Evaluation of the Safe Water System in Jolivert Haiti by Bacteriological Testing and Public Health Survey. Department of Civil and Environmental Engineering. Cambridge, MA, USA, Massachusetts Institute of Technology. MEng.
CARE (Undated). Global Development Alliance, Safe Drinking Water Alliance, Report of Findings: Draft Outline. Atlanta, GA, USA, CARE.
CDC. (2008, 2008). “Effect of chlorine in inactivating selected microorganisms.” from http://www.cdc.gov/safewater/about_pages/chlorinationtable.htm.
Clasen, T. and S. Boisson (2006). “Household-Based Ceramic Water Filters for the Treatment of Drinking Water in Disaster Response: An Assessment of a Pilot Programme in the Dominican Republic.” Water Practice and Technology.
Clasen, T., J. Brown, et al. (2004). “Safe household water treatment and storage using ceramic drip filters: a randomised controlled trial in Bolivia.” Water Sci Technol 50(1): 111-5.
Clasen, T., S. Cairncross, et al. (2007). “Cost-effectiveness of water quality interventions for preventing diarrhoeal disease in developing countries.” J Water Health 5(4): 599-608.
Clasen, T., W. P. Schmidt, et al. (2007). “Interventions to improve water quality for preventing diarrhoea: systematic review and meta-analysis.” BMJ 334(7597): 782.
Clasen, T. and L. Smith (2005). The Drinking Water Response to the Indian Ocean Tsunami, including the Role of Household Water Treatment. Geneva, Switzerland, World Health Organization.
Clasen, T. F. and A. Bastable (2003). “Faecal contamination of drinking water during collection and household storage: the need to extend protection to the point of use.” J Water Health 1(3): 109-15.
Clasen, T. F., H. Thao do, et al. (2008). “Microbiological effectiveness and cost of boiling to disinfect drinking water in rural Vietnam.” Environ Sci Technol 42(12): 4255-60.
Colindres, R. E., S. Jain, et al. (2007). “After the flood: an evaluation of in-home drinking water treatment with combined flocculent-disinfectant following Tropical Storm Jeanne — Gonaives, Haiti, 2004.” J Water Health 5(3): 367-74.
Colwell, R. R., A. Huq, et al. (2003). “Reduction of cholera in Bangladeshi villages by simple filtration.” Proc Natl Acad Sci U S A 100(3): 1051-5.
Crump, J. A., G. O. Okoth, et al. (2004). “Effect of point-of-use disinfection, flocculation and combined flocculation-disinfection on drinking water quality in western Kenya.” J Appl Microbiol 97(1): 225-31.
Doocy, S. and G. Burnham (2006). “Point-of-use water treatment and diarrhoea reduction in the emergency context: an effectiveness trial in Liberia.” Trop Med Int Health 11(10): 1542-52.
Dunston, C., D. McAfee, et al. (2001). “Collaboration, cholera, and cyclones: a project to improve point-of-use water quality in Madagascar.” Am J Public Health 91(10): 1574-6.
EHP. (2008). “Point-of-use Water Treatment Bibliography.” from www.ehproject.org/ehkm/pou_bib2.html.
Gupta, S. K., A. Suantio, et al. (2007). “Factors associated with E. coli contamination of household drinking water among tsunami and earthquake survivors, Indonesia.” Am J Trop Med Hyg 76(6): 1158-62.
Hoque, B. A. and S. Khanam (Undated). Efficiency and Effectiveness of Point-of Use Technologies in Emergency Drinking Water: An Evaluation of PUR and Aquatab in Rural Bangladesh Dhaka, Bangladesh, Environment & Population Research Centre.
Kaiser, N., K. Liang, et al. (2002). Biosand Filter: Summary of all lab and field tests., Samaritan’s Purse.
Kotlarz, N., D. S. Lantagne, et al. (Submitted). “Turbidity and chlorine demand reduction using locally available physical water clarification mechanisms before household chlorination in developing countries.” J Water Health.
Lantagne, D. S. (2001). Investigations of the Potters for Peace Colloidal Silver Impregnated Ceramic Filter. Report 1: Intrinsic Effectiveness. Allston, MA, USA, Alethia Environmental.
Lantagne, D. S. (2001). Investigations of the Potters for Peace Colloidal Silver Impregnated Ceramic Filter. Report 2: Field Investigations. Allston, MA, USA, Alethia Environmental.
Lantagne, D. S. (in press). “Sodium hypochlorite dosage for household and emergency water treatment.” Journal of the American Water Works Association.
Lantagne, D. S., R. Quick, et al. (2008). “Disinfection by-product formation and mitigation strategies in point-of-use chlorination of turbid and non-turbid waters in western Kenya.” J Water Health 6(1): 67-82.
Lantagne, D. S., R. Quick, et al. (2006). “Household water treatment and safe storage options in developing countries: a review of current implementation practices.” Woodrow Wilson International Center for Scholars’ Environmental Change and Security Program.
Mendez-Hermida, F., J. A. Castro-Hermida, et al. (2005). “Effect of batch-process solar disinfection on survival of Cryptosporidium parvum oocysts in drinking water.” Appl Environ Microbiol 71(3): 1653-4.
Mong, Y., R. Kaiser, et al. (2001). “Impact of the safe water system on water quality in cyclone-affected communities in Madagascar.” Am J Public Health 91(10): 1577-9.
Palmer, J. (2005). Community acceptability of household ceramic water filters distributed during Oxfam’s response to the tsunami in Sri Lanka. London, UK, London School of Hygiene and Tropical Medicine. MSc.
Preston, K., D. S. Lantagne, et al. (In writing). “Turbidity and chlorine demand reduction using locally available chemical water clarification mechanisms before household chlorination in developing countries.”
Quick, R. E., L. V. Venczel, et al. (1999). “Diarrhoea prevention in Bolivia through point-of-use water treatment and safe storage: a promising new strategy.” Epidemiol Infect 122(1): 83-90.
Rainey, R. C. and A. K. Harding (2005). “Drinking water quality and solar disinfection: effectiveness in peri-urban households in Nepal.” J Water Health 3(3): 239-48.
Ritter, M. (2007). Preliminary Report: Determinants of Adoption of Household Water Treatment in Haiti Jolivert Safe Water for Families(JSWF) Program. Atlanta, GA, USA, Emory University.
Roberts, L., Y. Chartier, et al. (2001). “Keeping clean water clean in a Malawi refugee camp: a randomized intervention trial.” Bull World Health Organ 79(4): 280-7.
Sobsey, M., C. E. Stauber, et al. (2008). “Point of use household drinking water filtration: A practical, effective solution for providing sustained access to safe drinking water in the developing world.” Environ Sci Technol 42(12): 4261-7.
Souter, P. F., G. D. Cruickshank, et al. (2003). “Evaluation of a new water treatment for point-of-use household applications to remove microorganisms and arsenic from drinking water.” J Water Health 1(2): 73-84.
SP (2006). PUR-Purifier of Water IDP Camp Distribution Program, LIra District, Northern Uganda, Project End Report. Boone, NC, USA, Samaritan’s Purse.
SPHERE (2004). Humanitarian Charter and Minimum Standards in Disaster Response. Geneva, Switzerland, The Sphere Project.
Walden, V. M., E. A. Lamond, et al. (2005). “Container contamination as a possible source of a diarrhoea outbreak in Abou Shouk camp, Darfur province, Sudan.” Disasters 29(3): 213-21.
Compiled initially by Lucy Staveley, October 2007. Revised and expanded by Daniele Lantagne, July 2008.
Reference:
Lantagne, D and Stavely L. (2008) Oxfam Houshold Water Treatment Technical Brief. Oxfam International, Oxford, UK.
